Professor Mike English

Contact information
Podcast interviews
Hospitals and Health for All?

Health Systems Collaborative focuses on improving healthcare delivery for low-income populations in Africa, especially in hospitals in rural areas. The AFRHiCARE project, a collaboration with clinicians, social scientists, and economists in Uganda, Kenya, South Africa and Oxford, examines how hospitals can effectively utilise technologies and innovations. We aim to optimise hospital operations to deliver high-quality care, ensuring essential services for patients in resource-poor settings across Africa.
Health services that deliver for newborns

Basic hospital care may be key to saving newborn lives. Professor Mike English outlines a multidisciplinary project engaging policy-makers and practitioners in Kenya. This project demonstrated poor coverage of Nairobi’s 4.25 million population if a sick newborn baby needs quality hospital care. Using novel research approaches the team also identified how severe shortages of nurses contribute to poor quality of care for patients and negatively affect nurses themselves. This interview was recorded in 2018
Colleges
Mike English
Professor of International Child Health
- Leader of the Health Systems Collaborative (HSC)
Visit HSC pages
Health Services Research
Mike English is a UK trained paediatrician who worked in Kenya for 25 years supported by a series of Wellcome fellowships. In Kenya he worked as part of the KEMRI-Wellcome Nairobi Programme and built up the Health Services Unit in collaboration with the Ministry of Health, the University of Nairobi and a wide set of national and international collaborators. His work focuses predominantly on improving care in African District Hospitals, often takes Child and Newborn Health as a focus, but increasingly tackles health services or wider health systems issues affecting quality of care. Mike now co-leads the Health Systems Collaborative in Oxford which is part of the NDM-Centre for Global Health Research.
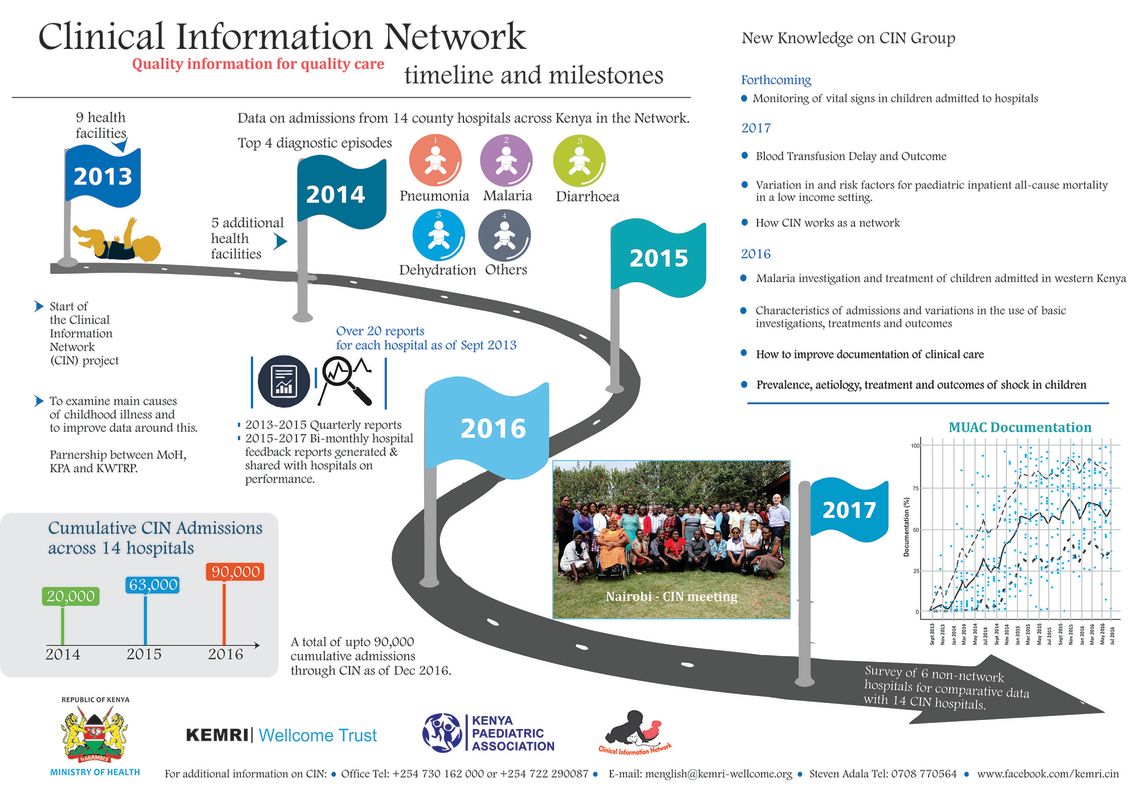
Mike continues to work closely with Kenyan colleagues on a range of projects. He initiated the Kenyan Clinical Information Network (CIN) in 2013 and further developed this platform over 10 years as an example of a low-cost learning health system. The CIN now spans 24 Kenyan hospitals and supports multiple clinical, implementation and improvement projects as well as a wide set of health services and systems research. Methods employed span: clinical epidemiology including developing national, evidence-based guidelines, clinical trials and some of the largest hospital based observational studies in Africa; mixed methods implementation research, health workforce research including work on task-sharing (eg. HIGH-Q) and professionals' training and careers and wider systems research on qualitative studies of families' and health workers' experiences and service redesign. New collaborations are helping to extend the forms of health services / health systems research in Vietnam, Burundi, UK and Ghana with a strong focus on capacity building of LMIC scientists.
For many years Mike has provided technical advice to the Kenyan government and WHO on a range of issues related to child and newborn survival and health systems performance. He is currently serving on a number of expert committees including the Strategic and Technical Advisory Group of Experts for Maternal, Newborn, Child and Adolescent health and nutrition and was a member of the Lancet Global Health Commission on High Quality Health Systems in the SDG Era.
Recent publications
The normalisation of under-resourcing limits the potential for improvement of critical care: evidence from a multi-method study of Kenyan hospitals
Journal article
McKnight J. et al, (2026), Social Science & Medicine, 396, 118843 - 118843
A framework and practical approach to identify and address ethical issues arising in interventional health systems research
Journal article
Mutua E. et al, (2026), International Journal of Nursing Studies, 174, 105263 - 105263
Implementing a change process to support respectful communication in newborn units in Kenya: A qualitative study.
Journal article
Boga M. et al, (2026), International journal of nursing studies, 173
Applying a multi-layered, mixed methods approach to evaluate technology and workforce interventions in Kenyan neonatal units
Journal article
Maina M. et al, (2025), Global Health Action, 18
Developing and integrating physician assistants/associates in UK hospital teams: a realist review of lessons from international experiences
Journal article
Zhao Y. et al, (2025), BMC Medicine, 23